Adopting new technologies usually requires some adjustments to routines and care pathways due to factors such as heavy workloads, changes to clinical workflows, concerns about data security and patient privacy and issues of interoperability across different information systems. This is why pilot programmes can provide invaluable insights that later support large-scale adoption (as covered in the Evaluation Phase).
Normalisation Process Theory
Challenges can be overcome by following a structured and iterative approach to the scaling and adoption of digital therapies in the NHS and other healthcare settings. One of these is Normalization Process Theory (NPT) which is a framework for identifying the factors that promote or hinder the integration of new interventions and solutions, including digital therapies into routine practice. NPT highlights three key challenges: implementing practices and bringing them into action; embedding practices into everyday workflows; and integrating practices within the social structures of an organisation.
NPT sets out four core mechanisms. Their implementation begins during the initial pilot phases (as covered in previous sections) and requires tailoring to the specific NHS organisation involved. As adoption is scaled, the processes are further refined to suit different types of NHS settings.
1. Coherence: How staff understand and make sense of the new digital therapy
- Do staff understand the purpose of the product?
- How do they perceive the value of the product for the service and for patients?
- Do they understand what tasks the intervention requires of them?
2. Cognitive participation: How staff promote the digital therapy
- Do the stakeholders believe they are the right people to drive forward the implementation?
- Do they agree that promoting the digital therapy is part of their work?
- Has the developer created appropriate manuals and training opportunities for staff?
3. Collective action: How staff work to enact the therapy into practice
- Do those implementing the intervention have the correct skills and training for the job?
- Are there clear processes that allow staff to offer the digital therapy to patients and access the data it collects?
- Are there trained champions that are able to support staff in everyday practice?
- Do local and national resources and policies support the implementation of the digital therapy?
4. Reflexive monitoring: What is the impact of the new digital therapy and how can its practice be adjusted when it is in use?
- How are the stakeholders able to appraise the effectiveness of the intervention?
- How will individual users judge the effectiveness of the intervention?
- Are there processes to modify the intervention based on evaluation and experience?
Data collection and evaluation
An evidence-based approach is at the core of the medtech pathway and this continues through the phase of scaled adoption. Monitoring uptake across NHS organisations relies on comprehensive data collection and achieving this at scale requires investment to establish a centralised system that enables consistent reporting and informed decision-making. Interoperability with NHS systems is a fundamental area that developers need to focus on, as it supports reliable and consistent data collection processes.
For example the Outcome and Registries Programme includes digital patient-reported outcome measures and patient-reported experience measures across . At this stage, the registry mainly focuses on high-risk implantable medical devices, such as pelvic floor mesh implants, cochlear implants, and trauma-related medical procedures. Patient panels contribute to practical areas such as data security, programme transparency and the development of public and patient information.
The figure below summarises the medtech strategy initiatives within the innovation pathway stages that support a data-driven approach:
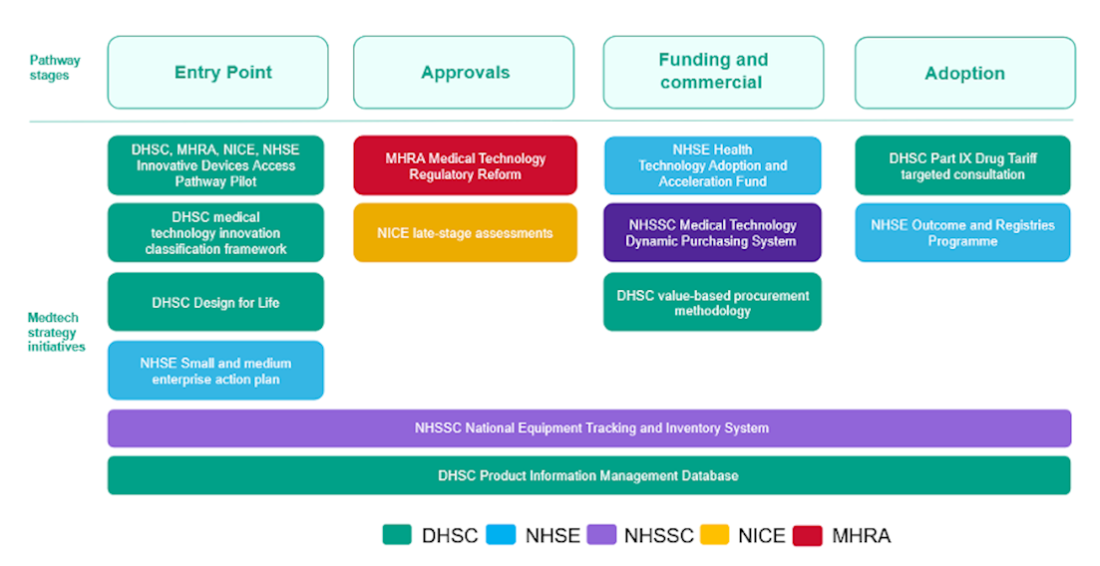
As discussed in the Commercialisation phase, a key challenge for developers is the absence of a centralised procurement system for digital therapies, which makes scaling adoption across NHS organisations more complex. The Department of Health and Social Care 10-Year Health Plan aims to address this challenge by creating a new “HealthStore”, which will be procured and funded centrally.
Tips and Resources
- To encourage adoption and uptake, it is important to identify the right champions among NHS staff who can advocate for the benefits of the digital therapy among colleagues and senior leaders. Building these relationships should start early, during pilot evaluations and initial data collection.
- Here is a summary of key questions for developers to consider in order to optimise the adoption and uptake of digital therapies:
- Where will it sit within the care pathway? Who needs to be aware of it?
- How will users find out about your product?
- If users are patients and they are referred by healthcare professionals, healthcare professionals need to: Understand the product and its value, align with what it’s trying to do, and be involved in its development or set-up.
- How will the product be introduced?
- If users sign up directly, think about recruiting /marketing avenues ahead of time.
- Will clinicians be supporting patients using the app?
- Will it require training and regular refreshers?
- What are the best adoption and implementation metrics? Adoption refers to the proportion and representativeness of settings and staff that are willing to initiate a program. Implementation refers to how well the intervention is being carried out.
- Look at the RE-AIM framework to identify the most appropriate ways to evaluate how well the digital intervention works in real-world settings.
Taking part in initiatives such as the Early Value Assessment (EVA), which provides a conditional recommendation for use in the NHS, can facilitate further evidence of patient and system outcomes, and better market adoption ahead of full NICE guidance. It can also serve as a “bridge” to a NICE MTG appraisal.

